You’ve Been Told to ‘Feed a Cold.’ Turns Out, Eating May Truly Boost Your Immune System Cells, According to a New Study
T cells, which target infection and disease, can become more effective after a meal. The finding might help improve cancer-fighting therapies and optimize our response to vaccines
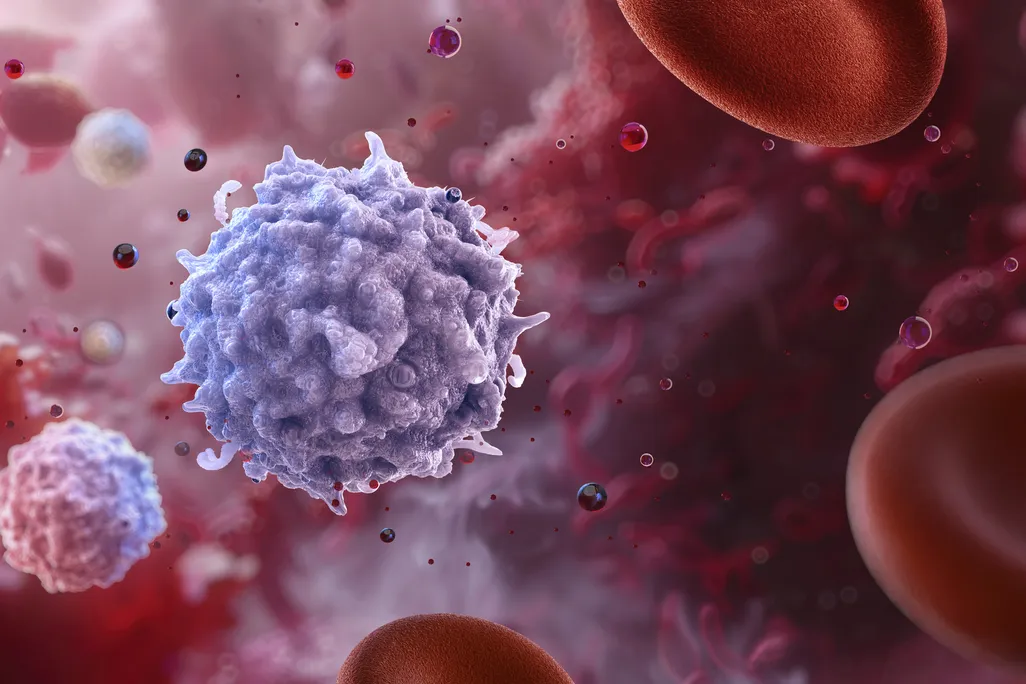
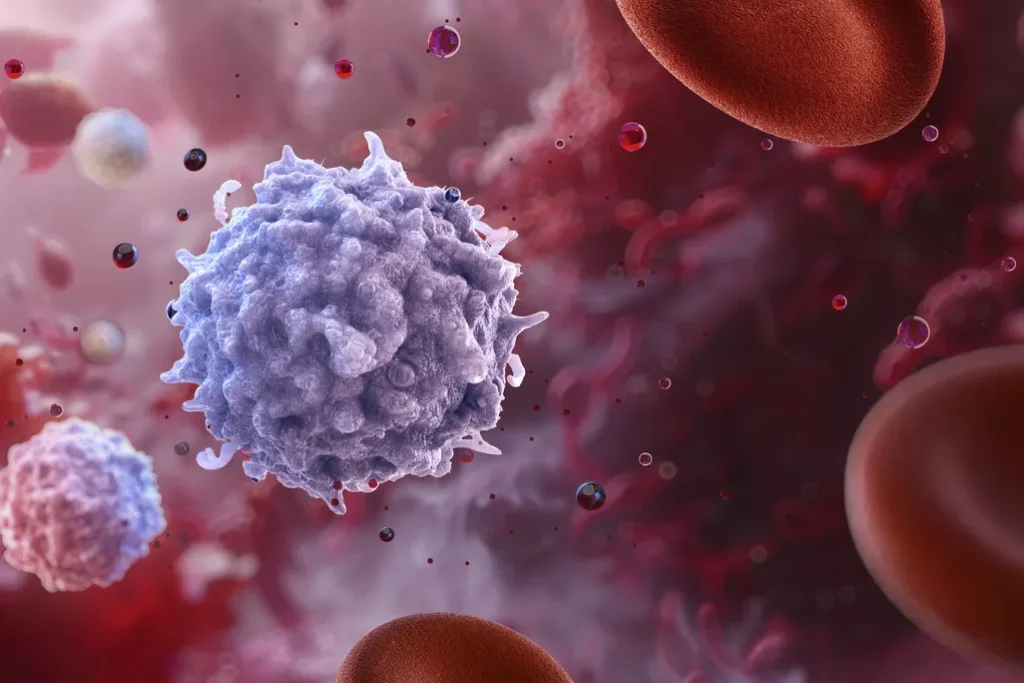
An illustration of lymphocytes, or white blood cells in the immune system, which include T cells and other disease-fighting cells
Ruslanas Baranauskas / Science Photo Library via Getty Images
When you’ve felt under the weather, you may have received the old advice: “Feed a cold, starve a fever.”
In certain ways, this adage isn’t true. No matter whether you have a fever or a cold, doctors advise drinking lots of fluids and maintaining good nutrition. The phrase has roots in an outdated idea that food can “warm” your body during a cold, and fasting can “cool it down” during a fever, as Lindsey Bever wrote for the Washington Post in February. It’s also not very clear—when you consider that a body fighting off illness can experience a fever and a cold at the same time, the saying’s meaning gets even more bungled.
Maybe better words to live by, as a new study suggests, are to feed both a fever and a cold.
According to a paper published last week in the journal Nature, eating meals appears to come with an immediate immune benefit. After participants had consumed breakfast and lunch, their infection-fighting cells showed a notable boost. The work could have implications for strengthening the immune system at key times, such as when receiving a vaccination, or combating autoimmune conditions.
“I think this is really an exciting study,” Lionel Apetoh, an immunologist at Indiana University who was not involved in the research, tells Nature’s Nick Petrić Howe.
Stronger immune cells in mice and humans
The researchers tested how eating affects the immune system’s T cells, a type of white blood cell that is key to staving off disease. When a pathogen enters the body, the immune system identifies the specific T cell primed to fight that kind of intruder, and the cell then multiplies into a legion of protective warriors that can vanquish the threat.
Scientists drew blood from 31 healthy volunteers at two times of day: first in the morning, after they had fasted overnight, and again six hours later, after they had eaten breakfast and lunch. They looked at the T cells in each blood sample and found that those from the later blood draw—the cells that had been fed—were better prepared to fight infections.
“It’s not like the fasted T cells don’t work. It’s just that fed T cells always win when we compare them head-to-head,” senior author Greg Delgoffe, an immunologist at the University of Pittsburgh, tells Asher Jones in a university statement. The fed cells were better at responding to infections, and they had metabolic advantages that helped them access the energy needed to mount a strong immune response.
Did you know? Lymphocytes in the immune system
- T cells belong to a class of white blood cells known as lymphocytes, and the other main type of lymphocytes in the body are B cells.
- While T cells fight pathogens and oversee the immune system’s response to invaders, B cells generate infection-fighting antibodies—as many as 2,000 per second.
The team also ran a similar test in mice, measuring their T cell activity after a meal or a fast. These experiments showed the same result—the animals’ cells had more massive mitochondria, more fat reserves and a greater ability to take up sugars post-eating. Some of those cells responded better to infections even seven days later.
The mice also demonstrated a longer-term benefit from a certain subset of T cells called memory cells. These special T cells remember pathogens the body has previously faced and rapidly respond, should these threats be encountered again. In the rodent experiments, fed mice produced more memory cells compared with the mice that had fasted, according to Nature.
From the mouse research, the team found that a fat-rich diet worked better than a diet rich in carbohydrates or protein when it came to boosting T cells. Specifically, the mice fed corn oil showed the strongest response—but that doesn’t mean a fatty meal will revitalize the human immune system. “We don’t want somebody out there just chugging a gallon of corn oil,” Delgoffe says to Scientific American’s Jackie Flynn Mogensen.
Fats worked for the mice, but as for the human participants, the contents of their meals were not regulated—they were allowed to eat whatever they wanted for breakfast and lunch. In one sense, that could be a limitation of the research, as Apetoh notes to Nature; it means scientists can’t discern which specific nutrients might have been responsible for giving the T cells a boost. But taken another way, this lack of control for meals suggests the study’s results are wide-reaching. “What we were able to say was it happened every time,” Delgoffe tells Nature; they observed the heightened T cell response regardless of the meal eaten.
Potential benefits for treating disease
Most research on human immunity does not take into account whether participants have recently eaten, according to the paper, so the work offers a new consideration for future studies.
“This highlights a massive, previously overlooked factor in medical research and vaccine efficacy,” says co-author Alok Kumar, an immunologist at the University of Pittsburgh, in the statement.
The findings also have implications for immune-related treatments, such as chimeric antigen receptor T-cell therapy, or CAR T-cell therapy, used to combat some cancers. The process removes T cells from a patient, adds a lab-made gene to make them stronger against fighting cancer and replaces them via infusion into the blood.
“This tells us that if you’re going to get vaccinated or if you’re getting blood drawn to collect T cells for CAR-T therapy, you might want to do it after lunch,” Delgoffe says in the statement.
In mouse tumor models, CAR-T cells derived from human T cells that were collected after eating showed better tumor control than those from T cells collected after a fast, per another statement.
Finally, the research points to chylomicrons—spherical particles that carry fats through the bloodstream—as the fuel for enhanced T cells after a meal. Reducing chylomicron activity, Delgoffe suggests in the statement, could help calm T cells in patients with autoimmune conditions, in which an overactive immune system attacks the body. And generating chylomicrons through diets, he speculates, may have the potential to improve outcomes during immunotherapy.
More research is needed to explore all of these ideas, and at this phase, the work doesn’t mean anyone should change how they eat. It doesn’t suggest that eating can treat diseases, and it doesn’t suggest that cancer patients should adjust their diets. But it does point to avenues for future study and the overall importance of healthy foods for giving our pathogen-fighting cells a key boost.
“We’re very, very excited about where things are going next,” Delgoffe tells Scientific American.